Doctors used IVF to create the first UK baby with DNA from three individuals to avert terminal disorders.
The HFEA reported “less than five” infants delivered using the approach. For privacy, none have been disclosed.
Assuming the method is safe and effective, more such births in the UK and elsewhere are likely in the coming years.
Why do couples employ this method?
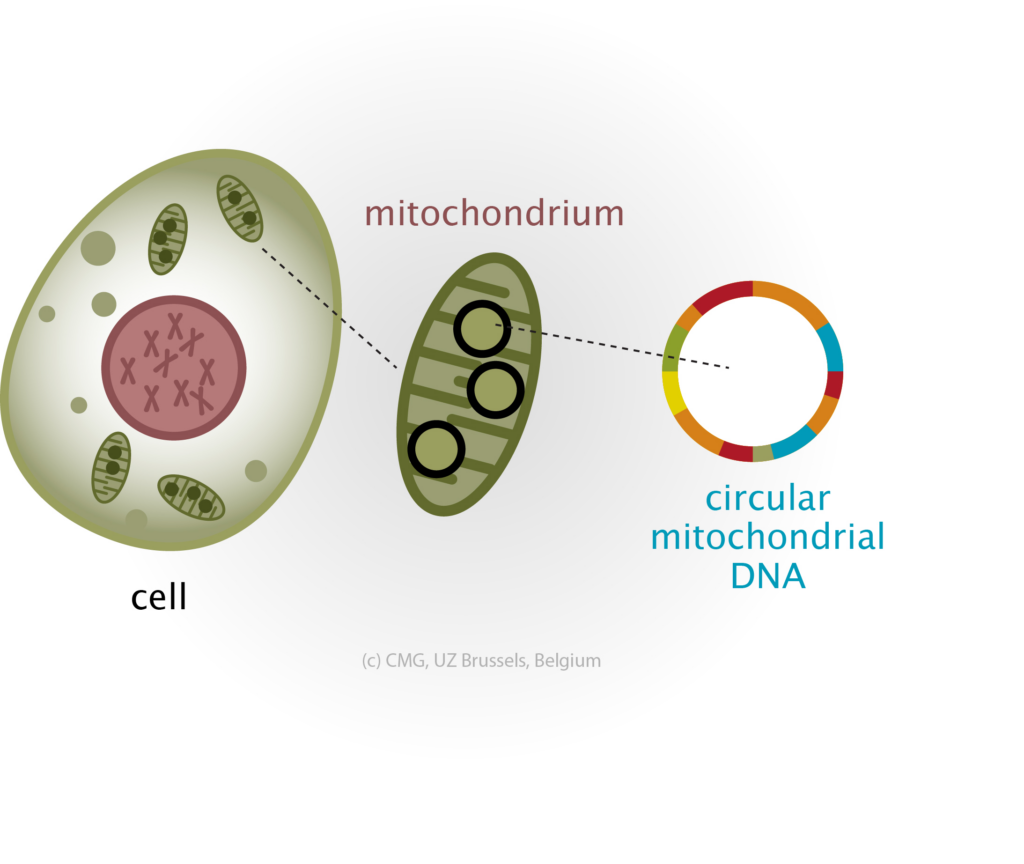
Mitochondrial donation therapy (MDT) prevents mothers from transferring faulty mitochondrial DNA to their children.
Cells’ batteries, mitochondria, inhibit normal development if they don’t operate.
What’s MDT?
MDT creates IVF embryos without dangerous mutations from healthy female donor eggs.
First, sperm from the father fertilizes eggs from the afflicted mother and a healthy female donor.
Next, the donor’s “nuclear” genetic material is replaced with the couple’s fertilized egg.
The egg has both parents’ chromosomes and the donor’s healthy mitochondria, not the mother’s.
MDT embryos mix the biological parents’ sperm and egg with the donor’s mitochondria.
Implanted in the womb.

How much third-parent DNA is in the baby?
Most of the child’s DNA, including personality and eye color, comes from the parents.
The “third parent” will supply a little quantity of mitochondrial DNA.
Mitochondria contain only 0.1 percent of a person’s DNA—37 genes—which are always inherited from the mother. The infant officially has three parents, but it is the product of two, and that 0.1 percent of genetic material is crucial to its health.
The second woman’s DNA only impacts mitochondria, not other essential features in the child.
Mitochondrial diseases—how serious?
Mitochondrial disorders affect 1 in 6,000 newborns.
These hereditary, inherited illnesses develop when mitochondria fail to provide energy for cells. These diseases are deadly.
Poor development, muscular tone, weakness, spasms, and a progressive decline in children are signs.
MDT is the sole hope for some families who have lost many children to hereditary mitochondrial disorders.

Who may receive MDT?
Treatment may be available for parents at high risk of passing on significant mitochondrial illness.
The HFEA recommends contacting a GP or Newcastle Fertility Centre at Life, the only national center licensed to research and treat patients using the procedure.
Mitochondrial donation therapy must be HFEA-approved to assure legality and ethics.
Scientists think the treatment may help 150 women a year, and many have expressed interest.
Do mitochondrial donors have parental rights?
No. The kid born through mitochondrial donation treatment will not be genetically related to the donor. The mitochondria contributes just 1% of the child’s DNA.
The donor stays nameless and has no legal rights over the kid.
From 16, the child can get certain mitochondrial donor information without identifying the donor.
The donor may include a personal description, medical history, and any other information they’ve consented to share with the kid.
UK MDT leader?
In 2017, the HFEA cautiously approved mitochondrial replacement therapy (MRT) at the Newcastle Fertility Centre, making Britain the first country to do so.
Mexico had the first three-parent baby in 2016, despite lax regulations.
HFEA has approved at least 30 UK instances on a case-by-case basis.
Concerned about patient confidentiality, Newcastle clinic doctors have not revealed MDT birth details. following a Guardian freedom of information request, the HFEA revealed that a few UK infants have been delivered following MDT.
Is MDT safe and effective?
The method is risky and the health of UK infants born using it is unknown.
Scientists, regulators, and medics will closely monitor these newborns when data becomes available.
The little number of defective mitochondria transferred over from the mother’s egg to the donor egg can grow in the pregnancy, according to previous study. Reversion or reversal may cause child illness.
Why some MRT-born children’s cells reverse and others don’t is unknown. Monkeys and mice showed that such newborns would likely be healthy, but humans may not.
What follows?
Experts will examine evidence carefully. “The HFEA continues to review clinical and scientific developments for mitochondrial donation treatment,” stated Peter Thompson, HFEA CEO.
“Passed only after many years of careful research, assessment and deliberation,” said Progress Education Trust head Sarah Norcross of UK treatment legislation.
The next stage in the gradual and careful process of examining and improving mitochondrial donation is the birth of a few UK newborns with donated mitochondria.
“While knowing that babies have been born in the UK following the use of mitochondrial replacement techniques is newsworthy, especially as this is being done in an appropriately regulated environment, scientists, clinicians and patients will want to see the details,” said Francis Crick Institute Professor Robin Lovell-Badge.
“These will be published, probably in a peer-reviewed scientific journal, hopefully soon. The Newcastle team was careful and sought to include some follow-up data on the newborns while safeguarding the families’ anonymity. It’s difficult.”
“It will be interesting to see how well the MRT technique worked in practice, whether the babies are free of mitochondrial disease, and whether they are at risk of developing problems later in life or, if female, if their offspring are.
“Such problems might arise if there is ‘reversion’, where the initially small amounts of the mother’s mitochondrial DNA, with the disease-causing variant gene, are carried over with her nuclear DNA and amplified.”

